Xanax vs Valium vs Ativan vs Klonopin: Key Differences
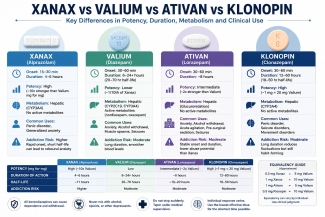
Xanax, Valium, Ativan, and Klonopin are the four most commonly prescribed benzodiazepines in the United States. All four work by enhancing the activity of gamma-aminobutyric acid — a neurotransmitter that slows down the central nervous system — but they are not interchangeable. They differ in how quickly they take effect, how long they last, how potent they are milligram for milligram, what conditions they are prescribed for, and how likely they are to cause dependence.
Understanding these differences matters because benzodiazepine prescriptions continue to rise, misuse is widespread, and withdrawal from these medications can be medically dangerous. This guide compares all four drugs across the dimensions that matter most — for prescribers, for patients, and for families trying to understand what their loved one is taking.
What Are Benzodiazepines and How Do They Work
Benzodiazepines are a class of central nervous system depressants that bind to GABA-A receptors in the brain. When GABA activity increases, neural firing slows down. The result is reduced anxiety, muscle relaxation, sedation, and in some cases anticonvulsant effects. All benzodiazepines produce these effects — but the degree of each effect, the speed of onset, and the duration of action vary significantly between individual drugs.
The structural differences between alprazolam (Xanax), diazepam (Valium), lorazepam (Ativan), and clonazepam (Klonopin) determine how each drug is absorbed, how it is metabolized by the liver, whether it produces active metabolites, and how long it stays in the body. These pharmacokinetic differences are what make one benzodiazepine better suited for panic attacks, another for seizure disorders, and another for alcohol withdrawal.
Xanax vs Valium: Key Differences
Xanax (alprazolam) and Valium (diazepam) are both prescribed for anxiety, but they differ in almost every clinical dimension. Xanax is a high-potency, short-acting benzodiazepine. Valium is a lower-potency, long-acting benzodiazepine with a much longer half-life and multiple active metabolites.
Onset and duration
Both drugs reach peak blood concentration within one to two hours of oral administration. Xanax effects typically last four to six hours. Valium effects last approximately the same duration per dose, but its active metabolites — particularly nordiazepam and oxazepam — extend the total duration of pharmacological activity to 20 to 70 hours. In some patients, Valium and its metabolites can take up to six weeks to be fully eliminated.
Potency
Xanax is approximately ten times more potent than Valium on a milligram-for-milligram basis. Standard equivalency tables indicate that 0.5 mg of alprazolam produces effects roughly comparable to 5 mg of diazepam. This higher potency, combined with its rapid onset, is what makes Xanax particularly effective for acute panic — but also what makes it more prone to misuse.
FDA-approved uses
Xanax is approved for generalized anxiety disorder and panic disorder. Valium is approved for a broader range of conditions, including anxiety, alcohol withdrawal, muscle spasms, and seizures. Valium is also used off-label for vertigo, opioid withdrawal, cocaine intoxication, and serotonin syndrome.
Addiction and withdrawal risk
Both drugs carry significant dependence risk with regular use. However, Xanax is generally considered to have a higher addiction potential because of the speed-reward cycle — rapid onset produces quick relief, which reinforces continued use. Withdrawal from Xanax tends to be more abrupt and intense due to its short half-life, while Valium withdrawal develops more gradually because the drug and its metabolites leave the body slowly.
Ativan vs Valium: Key Differences
Ativan (lorazepam) and Valium (diazepam) are both used for anxiety and in clinical settings for alcohol withdrawal and procedural sedation. The most important clinical distinction between them is how they are metabolized.
Metabolism
Valium undergoes oxidative metabolism through the CYP2C19 and CYP3A4 enzyme systems in the liver, producing active metabolites that extend its effects. Ativan undergoes glucuronidation — a simpler metabolic process that does not produce active metabolites and is less affected by liver function, age, or drug interactions. This makes Ativan the preferred benzodiazepine for elderly patients, people with liver disease, and individuals taking multiple medications.
Clinical use
Ativan is frequently used in hospital settings for pre-surgical anxiety, acute agitation, and alcohol withdrawal management. Emergency departments often prefer Ativan because of its predictable pharmacokinetics and its availability in injectable form. Valium is more commonly prescribed for conditions requiring prolonged muscle relaxation or where its long duration of action is an advantage, such as seizure disorders or sustained alcohol withdrawal protocols.
Equivalency
One milligram of lorazepam (Ativan) is approximately equivalent to 5 mg of diazepam (Valium). Ativan has an intermediate onset — slightly slower than Xanax — and a duration of effect of approximately eight hours, making it longer-acting than Xanax but shorter-acting than Valium.
Xanax vs Ativan: Key Differences
Xanax and Ativan are both commonly prescribed for anxiety and are sometimes perceived as interchangeable. They are not. The differences in their pharmacokinetics affect how they are used clinically, how quickly dependence develops, and how they should be discontinued.
Speed of onset
Xanax generally takes effect within 15 to 30 minutes, making it one of the fastest-acting oral benzodiazepines. Ativan typically takes 30 to 60 minutes to reach full effect. For people experiencing acute panic attacks, this difference in onset can be clinically significant.
Duration of action
Xanax lasts approximately four to six hours per dose. Ativan lasts approximately eight hours. This longer duration means Ativan may require fewer daily doses for sustained anxiety management, while Xanax may need to be taken three or more times per day.
Metabolism and population differences
Xanax is metabolized by the CYP3A4 enzyme pathway, which can be inhibited by certain medications and by grapefruit juice. People of Asian descent achieve higher peak concentrations of Xanax and experience longer-lasting effects. Ativan's glucuronidation pathway is less susceptible to these interactions, making it more pharmacokinetically predictable across populations.
Abuse potential
Studies and clinical consensus suggest that Xanax has a somewhat higher potential for misuse than Ativan. The mechanism is straightforward — Xanax's rapid onset creates a more pronounced subjective "hit," which can reinforce compulsive use patterns. This does not mean Ativan is safe from misuse — all benzodiazepines carry dependence risk — but the distinction matters in prescribing decisions.
Klonopin vs Ativan vs Xanax: Key Differences
Klonopin (clonazepam) occupies a different position in the benzodiazepine class. It has a slower onset than Xanax or Ativan but provides the longest-lasting effects of the four drugs — six to twelve hours per dose — with a half-life of 18 to 50 hours.
What Klonopin is prescribed for
Klonopin is FDA-approved for seizure disorders and panic disorder. It is also used off-label for generalized anxiety, social anxiety disorder, and certain movement disorders. Its long duration makes it suitable for conditions requiring sustained control rather than rapid relief.
How Klonopin compares to Xanax
Klonopin takes longer to kick in — typically 30 to 60 minutes compared to Xanax's 15 to 30 minutes. But its effects last significantly longer, which means fewer daily doses and less of the peaks-and-valleys cycle that can reinforce dependence with short-acting drugs. For people with panic disorder who need daily prevention rather than as-needed rescue dosing, Klonopin is often preferred over Xanax. Equivalency tables indicate that 0.5 mg of clonazepam is roughly equivalent to 0.5 mg of alprazolam.
How Klonopin compares to Ativan
Klonopin lasts longer than Ativan and has stronger anticonvulsant properties. Ativan has a more predictable metabolism and fewer drug interactions. In practice, Klonopin tends to be used for long-term anxiety and seizure management, while Ativan is used more in acute or hospital settings.
Benzodiazepine Equivalency Chart
The following equivalencies are approximate guides used by clinicians when switching between benzodiazepines or calculating cross-taper doses. Individual variation — based on age, body composition, liver function, genetics, and concurrent medications — means these should never be used for self-dosing.
- Alprazolam (Xanax) 0.5 mg
- Diazepam (Valium) 5 mg
- Lorazepam (Ativan) 1 mg
- Clonazepam (Klonopin) 0.5 mg
These four doses are considered approximately equivalent in anxiolytic effect.
What Is Hydroxyzine and How Does It Compare to Benzodiazepines
Hydroxyzine (brand names Vistaril, Atarax) is not a benzodiazepine. It is a first-generation antihistamine that is sometimes prescribed as a non-addictive alternative for anxiety. Hydroxyzine works by blocking histamine H1 receptors, producing sedation and mild anxiolytic effects without the GABA mechanism, the euphoric potential, or the dependence risk associated with benzodiazepines.
Hydroxyzine is often prescribed for patients with a history of substance use disorder who should not take benzodiazepines, or as a bridge medication during benzodiazepine tapering. It is not as effective as benzodiazepines for acute panic or severe anxiety, but for mild to moderate generalized anxiety, it represents a meaningful alternative with a far better safety profile.
When Benzodiazepine Use Becomes a Problem
Benzodiazepines are intended for short-term use — typically two to four weeks. Dependence can develop within days to weeks of daily use. Tolerance — needing a higher dose to achieve the same effect — follows quickly. When someone increases their dose without medical supervision, takes a benzodiazepine more frequently than prescribed, obtains prescriptions from multiple providers, or combines benzodiazepines with alcohol or opioids, the pattern has crossed from medical use into misuse.
Signs of benzodiazepine dependence
- Needing a higher dose to feel the same effect
- Feeling anxious, agitated, or physically ill when a dose is missed
- Running out of a prescription early
- Combining benzodiazepines with alcohol, opioids, or other sedatives
- Continued use despite negative consequences at work, home, or in relationships
- Unsuccessful attempts to cut down or stop
Why benzodiazepine withdrawal is medically dangerous
Unlike opioid withdrawal, which is extremely uncomfortable but rarely fatal, benzodiazepine withdrawal can produce seizures, psychosis, and death. This is because GABA receptors have been down-regulated by chronic benzodiazepine exposure, and removing the drug suddenly leaves the brain in a hyperexcitable state. Withdrawal severity depends on which benzodiazepine was used (short-acting drugs produce more intense withdrawal), how long it was used, the dose, and whether other CNS depressants were involved.
Medical tapering — gradually reducing the dose under clinical supervision, often using a long-acting benzodiazepine like Valium as the tapering agent — is the standard of care for benzodiazepine discontinuation. Stopping cold turkey is not recommended under any circumstances for someone who has been taking benzodiazepines daily for more than a few weeks.
Treatment for Benzodiazepine Addiction
Treatment for benzodiazepine use disorder typically begins with medically supervised detox, where the drug is tapered gradually to prevent withdrawal complications. After detox, most individuals benefit from structured treatment — either inpatient rehab, partial hospitalization, or intensive outpatient programming — that addresses the underlying anxiety, trauma, or co-occurring conditions that led to benzodiazepine use in the first place.
Cognitive behavioral therapy, exposure therapy, and non-addictive pharmacological alternatives (including hydroxyzine, buspirone, and certain SSRIs) are the foundation of long-term recovery from benzodiazepine dependence.
For individuals and families on Long Island dealing with benzodiazepine dependence, Long Island Addiction Treatment Resources provides free, confidential treatment navigation — including clinical assessment, insurance verification, and placement into detox and rehab programs that specialize in benzodiazepine tapering and withdrawal management.
Frequently Asked Questions
Is Ativan the same as Xanax?
No. Ativan (lorazepam) and Xanax (alprazolam) are both benzodiazepines, but they differ in onset speed, duration of action, metabolism, and clinical use. Xanax acts faster and wears off sooner. Ativan lasts longer and is metabolized through a simpler pathway that makes it safer for elderly patients and those with liver issues.
What is the difference between Xanax and Valium?
Xanax (alprazolam) is a high-potency, short-acting benzodiazepine primarily used for anxiety and panic disorder. Valium (diazepam) is a lower-potency, long-acting benzodiazepine with a much longer half-life, used for anxiety, muscle spasms, seizures, and alcohol withdrawal. Xanax is approximately ten times more potent than Valium milligram for milligram.
Which is stronger, Xanax or Valium?
Xanax is more potent per milligram. A 0.5 mg dose of Xanax produces effects roughly equivalent to 5 mg of Valium. However, "stronger" does not mean "better" — the right choice depends on the condition being treated, the duration of effect needed, and the individual patient's metabolism and medical history.
What is the difference between Ativan and Valium?
Ativan (lorazepam) is metabolized through glucuronidation, which produces no active metabolites and is less affected by age, liver function, or drug interactions. Valium (diazepam) is metabolized through oxidative pathways and produces active metabolites that extend its effects for days. Ativan is preferred in hospital settings and for elderly patients. Valium is preferred for conditions requiring prolonged muscle relaxation or seizure control.
Is Klonopin stronger than Xanax?
They are approximately equivalent in potency — 0.5 mg of clonazepam is roughly equal to 0.5 mg of alprazolam. The key difference is duration. Klonopin lasts much longer (six to twelve hours versus four to six hours for Xanax), which means it provides more sustained anxiety control but takes longer to take effect.
What is Ativan used for?
Ativan (lorazepam) is FDA-approved for generalized anxiety disorder and short-term anxiety-related insomnia. It is also widely used in clinical settings for pre-surgical anxiety, acute agitation, alcohol withdrawal management, and procedural sedation. Its predictable metabolism makes it a preferred choice in emergency departments and for patients with compromised liver function.
What is the Ativan dosage for anxiety?
Typical starting doses of Ativan for anxiety range from 0.5 mg to 1 mg taken two to three times daily. Dosing should be individualized by a prescriber based on the severity of symptoms, patient age, body weight, and concurrent medications. Elderly patients typically require lower doses due to slower metabolism.
What is the generic name for Xanax?
The generic name for Xanax is alprazolam. Generic alprazolam is widely available and contains the same active ingredient at the same doses as the brand-name product.
What is the generic name for Ativan?
The generic name for Ativan is lorazepam. It is available in tablet and injectable forms.
What is diazepam?
Diazepam is the generic name for Valium. It is a long-acting benzodiazepine with a half-life of 20 to 70 hours, prescribed for anxiety, muscle spasms, seizures, and alcohol withdrawal. It produces active metabolites that extend its pharmacological effects well beyond the parent drug's duration.
What is clonazepam?
Clonazepam is the generic name for Klonopin. It is a long-acting benzodiazepine primarily prescribed for seizure disorders and panic disorder. It has a half-life of 18 to 50 hours and provides sustained anxiolytic and anticonvulsant effects.
What are benzodiazepines?
Benzodiazepines are a class of prescription medications that enhance the activity of GABA, a neurotransmitter that slows down the central nervous system. They are used to treat anxiety disorders, panic disorder, seizures, muscle spasms, insomnia, and alcohol withdrawal. All benzodiazepines carry risks of tolerance, physical dependence, and withdrawal with regular use.
Is hydroxyzine the same as a benzodiazepine?
No. Hydroxyzine is a first-generation antihistamine, not a benzodiazepine. It does not work on GABA receptors, does not produce euphoria, and does not carry the same dependence or withdrawal risks. It is sometimes prescribed as a non-addictive alternative for mild to moderate anxiety, particularly for patients with a history of substance use disorder.
Can you get addicted to Xanax or Valium?
Yes. All benzodiazepines carry a risk of physical dependence with regular use, even at prescribed doses. Dependence can develop within days to weeks. Xanax tends to have a higher addiction potential than Valium because its rapid onset and short duration create a pronounced cycle of relief and rebound that reinforces continued use.
How long does benzodiazepine withdrawal last?
Acute withdrawal typically lasts one to four weeks depending on the specific drug, duration of use, and dose. Short-acting benzodiazepines like Xanax produce withdrawal symptoms within hours of the last dose, peaking around day two to three. Long-acting benzodiazepines like Valium may not produce withdrawal symptoms for several days. Post-acute withdrawal symptoms — including anxiety, insomnia, and cognitive difficulties — can persist for months in some cases.
Is it safe to mix benzodiazepines with alcohol?
No. Combining any benzodiazepine with alcohol is dangerous. Both substances depress the central nervous system, and their combined effect can cause respiratory failure, loss of consciousness, aspiration, and death. The FDA has issued black box warnings on all benzodiazepines regarding concurrent use with opioids and other CNS depressants, and the same risks apply to alcohol.
What should I do if a loved one is dependent on benzodiazepines?
Do not encourage them to stop suddenly — abrupt benzodiazepine cessation can cause seizures and other life-threatening withdrawal complications. A medical taper under clinical supervision is the standard of care. For help navigating treatment options for benzodiazepine dependence, Long Island Addiction Treatment Resources provides free, confidential assessments and placement into detox and rehab programs that specialize in benzodiazepine withdrawal management.