UNODC Current NPS Threats
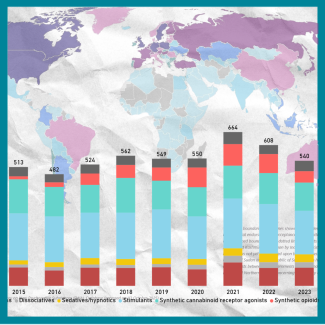
The UNODC Early Warning Advisory highlights a continued global expansion of new psychoactive substances (NPS), with nearly 1,400 substances reported worldwide. In 2024 alone, a record number of substances were identified, including over 100 newly detected compounds.
Synthetic opioids—particularly fentanyl analogues and nitazenes—are a growing concern, now reported across all regions. At the same time, benzodiazepine-type substances remain widely present in drug samples. A key emerging risk is polysubstance use, with a significant share of deaths involving multiple substances.
Overall, the...



